by Jess Helle-Morrissey, MA, MSW, LGSW, LCCE, CLEC
Nothing about my pregnancy went according to plan. After nearly 12 years of marriage and completion of my clinical social work graduate program, my husband Mitch and I decided it was finally time for us to start thinking about a family. Part of me always knew I’d have twins and so when I began dreaming of twins in the 5th week of my pregnancy, I had a feeling then that something magical was happening. And when I would talk to “baby” in my tummy, every cell in my body said, “That’s not right!” So I always talked to “babies” instead, just in case…
Each time we had a midwife appointment, Mitch would ask, “Can you tell if there are two in there?” (We have been together a long time – long enough for him to know that my intuition isn’t usually just a fluke.) My best friend was pregnant at the same time, due the same day, and I was consistently bigger than her, and MUCH sicker than her. I remember one day shopping for maternity clothes together – the two of us standing in front of the dressing room mirror and seeing how much bigger I was. I told her, “Look at my belly compared to yours. I think there are two babies in there.” She said, “Oh my god, can you imagine?!” In retrospect, I also started feeling movement around 12 weeks – like little ping pong balls bouncing around my belly – what my midwife referred to as an “early quickening”. So there were lots of signs backing up my intuition.
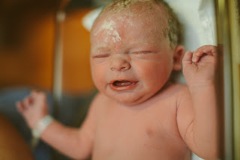
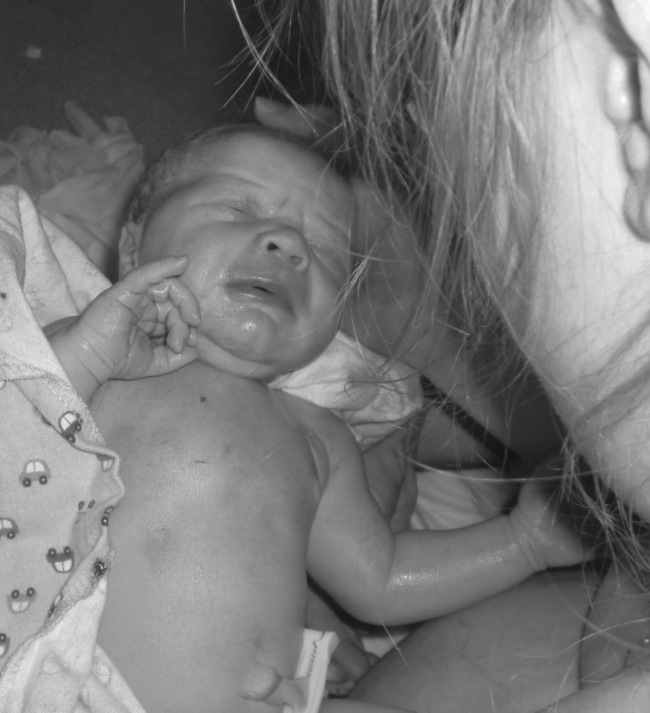
By the time our first ultrasound came around at 20 weeks, I told Mitch I was pretty sure they would find two babies. But I didn’t completely believe it yet – my heart knew it, but my head had not quite caught on. The ultrasound technician put the wand down on my belly and two perfect circles appeared on the screen. She immediately removed the wand, looked at us, and said, “Wait, is this your first ultrasound?” Thinking this was a standard question, I told her that it was. “Ahhhh, ok,” she said. She put the wand back down on my belly. “Because here’s a head, and here’s baby number two’s head.” Mitch immediately started laughing and I screamed and said, “I knew it!” The only place my intuition was off was that in my dreams, there was one boy and one girl. Instead, there were clearly two sweet identical little boys in there.

Our first glimpse of the babies! Two beautiful heads…
This was the first of many changes to how I imagined my birth would go. I’d been planning a home birth or a birth center birth and had been getting my care through a local birth center. My midwife told us they could not birth twins at the center due to their license. (No twins, no breech). She recommended an amazing OB in just over the border in Wisconsin. Kind of a drive, but totally worth it. Dr. H has the heart of a midwife, and I felt totally calmed to be working with him. He had a lot of experience with twins and was regarded as an expert on vaginal breech delivery – something that is fairly common with twins. “Breech is a perfectly valid way to come into the world,” he told me. I have never been afraid of unmedicated childbirth, but the idea of a hospital birth always scared me. Dr. H and this small community hospital were as close to a birth center as I would get this time around, and I knew it was the right place to get my care.
We certainly experienced some major “twinshock” – I spent the day after our ultrasound alternately laughing hysterically and crying hysterically. But once the news sunk in, we began to realize what an amazing miracle was taking place. Feeling the boys grow and move in my belly over the next few months was something I’ll never forget. As the months went by, I got bigger and bigger. I was measuring 40 weeks by 28 weeks pregnant, so… that was fun.

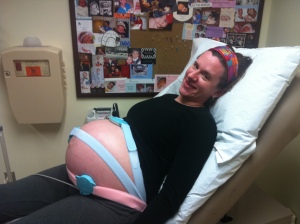
One of my final belly pictures, at 34 weeks…
Fast-forward to 34 weeks: I’d been feeling restless the past few days. I’d gotten up at 2 in the morning and taken a shower one night because I just had to. Mitch later told me that the late-night shower was when he started to think that the babies would be coming sooner than we thought – I’d never done anything like that. On a Thursday, I took a nap on the couch and woke up to a feeling that wasn’t quite right. Turns out I’d lost my mucus plug. I saw Dr. H the next day and he said not to worry – losing the mucus plug was a “nonspecific” sign. For the next few days, I started passing mucus regularly. Again, not necessarily anything to be concerned about. Still, we scheduled our second meeting with our doulas for that Monday just in case we were closer to the big show than we’d thought. Tuesday morning, I woke up with another feeling that a change had happened and found that I’d had some decent bloody show. We drove in to the L&D unit at our hospital and they put me on the fetal monitors, found that both babies looked good and saw that I was having some mild Braxton-Hicks contractions (which I’d been having since about 20 weeks). I was 80% effaced and 1-2 cm dilated, (within normal range for twins at my gestation) so they again weren’t worried. That was the first cervical check of my pregnancy.
 That night, some friends came over for a visit. In retrospect, I was having a low “restless” backache, and some intermittent crampiness in my thighs, but I chalked it up to the fact that I’d been laying on that hospital bed all day. I was in denial that I would go anything less than 40 weeks, so why would I think that labor would begin any time soon?
That night, some friends came over for a visit. In retrospect, I was having a low “restless” backache, and some intermittent crampiness in my thighs, but I chalked it up to the fact that I’d been laying on that hospital bed all day. I was in denial that I would go anything less than 40 weeks, so why would I think that labor would begin any time soon?
1:45 am, Wednesday 1/12/11: I was asleep and heard/felt a slight “pop!” and felt what seemed like a tidal wave of amniotic fluid rush out. (Good thing we’d just put the waterproof mattress pad down). Our joke now is that Mitch and half our bedroom furniture went rushing down the hall on the gigantic wave of amniotic fluid. Mitch woke to me saying, “Oh shit oh shit oh shit oh shit.” There was no mistaking what had just happened and it was too early. Just as Mitch asked me what was wrong, he started getting drenched and realized what was going on. He tells me now that he’ll never forget the sound of my voice when I woke him up that night.
Because I was 34 weeks and 4 days, it meant we couldn’t have the delivery at our Wisconsin hospital that we’d wanted, but my wonderful OB could catch our babies at a local hospital in the Twin Cities (ha!) with a NICU attached. Already one of my biggest labor fears was being realized: I’d be delivering in the most medicalized possible environment. Quite the change from my initial dream of a water birth at home. But I knew it was best for my early boys.
We called one of our doulas, who told me to take a shower, have a little meal, and take some time to breathe and reflect on the fact that I would meet my babies soon. She told me, “Check in with your babies, and let them know that it’s okay that they decided to be born today.” Until the day I die, I will remember those as some of the most powerful words ever spoken to me.
Mitch printed out my birth plan, put my labor playlist on my iPod, and made me some oatmeal. I sat on the couch in the dark and cried some tears – both happy and scared, and listened to a favorite song from my labor playlist,Djorolen, by Bela Fleck and Oumou Sangare. I hummed quietly to my boys and connected with them, and let them know that yes, it was okay that they decided to come earthside today. I didn’t remember it at the time but the translation of the lyrics to this song are, “The worried songbird cries out in the forest. Her thoughts go far away. For those of us who have no parents, her thoughts go to them.” I don’t think I fully understood the profundity and the sanctity of that moment at the time. In that moment, I was that worried songbird whose thoughts were far away. I felt worried, lost, happy, excited, calm – all at the same time. But from that moment on, there was no fear. I knew somehow that it would all be okay, that I would push both these babies out of my vagina with little problem, that my body knew how to do what needed to be done that day. Despite the fact that they were coming early, I knew deep down that they had chosen their birth day. I had total faith in my body and my babies.
About two hours from when my water broke, we were on our way to the hospital. By the time I got there at 4 AM (on all fours in the backseat, which felt GREAT), I’d begun having some mild contractions – nothing worse than period cramps. Our doulas Sarah and Amber met us in our labor room and we met Lori, our nurse for the day. Much to my pleasant surprise, she was totally accommodating of my natural birth plan – not wanting pain meds, epidural, or continuous fetal monitoring, etc. It really was the luck of the draw because depending on the nurse, she could have required continuous fetal monitoring due to hospital twin policy. She checked me and I was dilated to 4 cm. I couldn’t believe it – I’d barely felt a thing at that point.
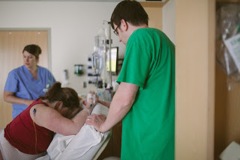
I spent the morning in the early labor phase doing lots of hip circles on the birth ball, doing squats and lunges, and yoga led by Sarah. This was where I was sooooo glad I’d gone to prenatal yoga classes during my pregnancy. I felt so strong and powerful. I was able to moan through contractions and recover my sense of humor and ability to converse in between. Both my doulas and Mitch had their hands on me almost all the time, which was exactly what I wanted – I felt so supported. I had my labor play list playing which was also tremendously comforting – it helped the small, sterile hospital space feel more like home.
Sometime around 10 or 11am, a distinct shift in my labor occurred. We’d been to a parent topic night at The Childbirth Collective called “The Natural Rhythm of Labor” where the presenter, an experienced doula, acted out the stages of labor in a very realistic manner. This proved to be one of the most helpful things throughout my labor because I sort of knew based on how I was acting where I was in the labor, and that how I was behaving was normal. I moaned, vocalized, and moved my body in a rhythm that came from deep within. Once I felt this shift, I knew we’d moved to the next level. I was beginning to feel tremendous downward pressure in my bottom and a need to bear down. The contractions were intense and I could no longer talk between them. I needed lots of help to not tense up with each contraction. Again, my doulas and Mitch were amazing in helping me to relax as best I could. Because of the urge to bear down, my favorite place for the rest of my labor was on the toilet in the dark bathroom. I spent some time in the tub, but it wasn’t very deep and didn’t provide the relief I’d hoped it would. While I was in the tub, our nurse checked me again and even though I was sure I was at about 28 centimeters dilated at that point, I was instead at 6.
We went back to the labor room and this was when I was beginning to tell my support team, “You guys, I don’t think I can do this anymore.” Again, I remembered from the Childbirth Collective class that this was a good sign because it meant I was getting closer to the end. “You ARE doing this!”, my support team reminded me. Eventually I began begging for an epidural – supposedly another sign that things were progressing. Sarah, Amber, and Mitch knew I didn’t want the epidural so they helped me through more contractions. All the while, I was saying I couldn’t do this anymore. I was so exhausted – I couldn’t understand why they wouldn’t just let me lay down in the bed! It was hard not to tense up so much, but Amber helped me do a low roar through my contractions. I also threw up several times at this point (sorry Amber!) – I again remembered from our Lamaze class that this was a “good sign”. Even deep in laborland, I was somehow able to remember that barfing was often an indicator of transition.

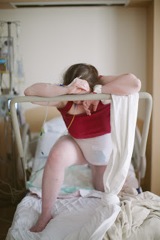
Amber and Mitch, helping me through a contraction…
The nurse checked me again because I was doing so much grunting in my contractions that she felt sure I was ready to push. She discovered that I was still at 6 cm, had a slight fever, and that my cervix was beginning to swell from all the downward pressure over the hours. Sarah and Amber had me switch my breathing technique so that I wouldn’t bear down so much, but it was nearly impossible not to. The nurse said, “Okay, I know you don’t want an epidural, but I think we need to do something to take the swelling out of your cervix.” There was part of me that wanted to look at my labor support team and say, “See!? I won! Epidural!” Even though I didn’t want it, the idea of relieving the intense pressure of the contractions had taken over. The anesthesiologist came in and as he was prepping me, he said, “I see you have some acne on your back. That can increase the potential for infection which can lead to paralysis and death.” I was like, “Yep, paralysis, death, got it. Sounds good. Let’s get that epidural now, please!”
After the epidural was placed, it took only about 10 minutes for a powerful realization to sink in: I was one of the small percentage of women the anesthesiologist mentioned during the informed consent for whom epidurals don’t work. The intensity of the contractions had only increased and I had full feeling and movement from the tips of my toes to the top of my head. I could have stood up and tap-danced, no problem. (If I knew how to tap-dance. Also, I did not feel like tap-dancing). Sarah and Amber sent Mitch to go get something to eat thinking that we’d have some time now that the epidural was in. Wrong – nurse checked me again since I was still vocalizing loudly, involuntarily bearing down, and clearly feeling the increasing intensity of each contraction. In retrospect, this was the final part of transition. The nurse informed me that I was at 10 centimeters – fully dilated and obviously pushing already.
Sarah called Mitch and told him to get back upstairs quickly. The nurse got scrubs for everyone (Twins automatically have to be delivered in the OR at most hospitals. Bummer.) And even though I was in a deep internal place, I knew we were at the end of my labor and the birth was near. I have never felt so fully in my body in my life – it was the most profound physical experience I think I’ll ever have. Sarah told me it would be okay if I started working with the pushes when my body felt like it. My OB was on his way from Wisconsin (at about 4pm – rush hour!) and I could tell the nurse was beginning to get a little nervous about who was going to catch these babies. Luckily, we rolled past Dr. H as they were wheeling me to the OR. Seeing his smile and thumbs-up was very reassuring. “You’re amazing!”, he called to me. “I’ll meet you in there!”
There were about 15 people in the OR – a team of NICU nurses for each baby plus the NICU resuscitation team, and some nurses for me. Mitch was at one side, my nurse at the other, and Sarah was at my head. Amber was taking pictures and videotaping. Side note: I’m SO glad my delivery was videotaped. I tell everyone to video their birth if possible. It was very healing for me to be able to watch what I did during the birth of my sons. It was tremendously empowering to be able to see the whole experience from a different vantage point. In the time since the birth, I’ve watched the video countless times, and I will show it to anyone who will watch it so they know the amazing things I am capable of. UPS guy? Thanks for the package, want to watch when I pushed two babies through my vagina without the aid of any pain medication?

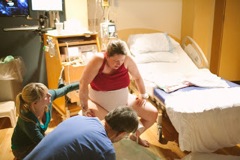
A doula’s support during pushing.
So anyway, pushing. I didn’t realize how much pushing a baby out feels like the exact same sensation as pooping. My pushing wasn’t super productive at first, but once Sarah started telling me to push into my bottom, it made all the difference. No wonder I’d wanted to sit on the toilet for the last several hours. At one point, I reached down and felt my little baby A’s head as I was pushing. That really helped me focus as well – there really and truly was a baby coming out of me! All this pushing wasn’t for nothing – I was moving that baby!
I was in such a deep internal place – a place I’ve never been before. Most everything just melted away and I had a singular focus that I wasn’t in control of. My body was doing the pushing and I was just along for the ride. My eyes were closed. I was aware of Sarah at my ear. I was aware of Dr. H’s kind and gentle encouragement. I was certainly aware of the intensity of the physical sensation. What I was most aware of, though, was my sweet Mitch at my left side. With each push I could hear his words of excitement, telling me I was amazing and telling me how each push got us a little closer to the end. I could hear the smile in his voice. I could tell he could see the progress I was making – our first baby’s head making more and more of an appearance with each push. I didn’t hear a trace of worry in his voice – only joy and amazement, and that more than anything else got me through.
After what felt like an eternity, but what was actually less than 40 minutes, Oskar Jeffrey was born at 5:09 pm, coming in at 4lb, 14oz and 18 inches long. O had a tough time at first – he was gray and floppy and did not cry for quite some time. They whisked him off to the NICU team as soon as Mitch cut the cord. Mitch went to Oskar, and Sarah told me to talk to him so he could hear my voice. He had to be intubated because he was having trouble breathing on his own. For whatever reason, I wasn’t able to do anything but watch – I could not find my voice in that moment. I’ll always be grateful to Sarah for being my voice when I could not speak, saying, “Oskar, honey! Hi, baby! You’re doing such a good job! We’re so glad you’re here!”
All of the sudden, I began to feel the urge to push again. I’d sort of forgotten that I had another baby in me. I heard Dr. H say, “There’s another bag of waters” and as he was saying that, my second bag of waters broke. When that happened, I heard him say, “And there’s a head!” Those were some of the sweetest words I’ve ever heard. My second little boy, who’d been breech the whole time in utero, had somehow managed to turn after his brother was born. I was honestly thinking, “I don’t know how I’m going to do this a second time.” But one contraction and about 3 pushes later, Henry Christopher entered the world head-first at 5:13pm, wriggling and crying. I barely felt him come out – all 5lb and 18 inches of him. They were able to put him on my chest for about 15 seconds and it was amazing – the biggest high of my life. I cried out, “Baby, baby, baby, baby, sweet baby! I’m your mom!” I felt an almost primal urge to lick him, and I wanted to kiss him nonstop. But he had to be intubated as well, so he was taken off pretty quickly also. “Just give a little push,” I heard Dr. H. say. And so I did, barely noticing I was delivering the enormous placenta that my boys had shared over the last eight months.

Moments after the boys were born. We did it.
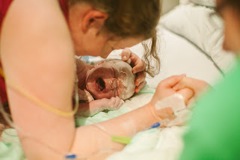
Meanwhile they’d stabilized the boys and were able to bring them to me briefly before transporting them to the NICU. I couldn’t believe how much I loved them. I kept saying over and over, “Mommy loves you so much.” It was scary seeing them with their ventilators in, but I had the feeling that everything would be alright. I knew they were in good hands. The same deep part of me that had known that I had twins in my belly from practically the moment the fertilized egg split into two also knew that they would be okay.
I was on such a high after the delivery. They wheeled me back to my room and right away I asked for the room service menu. I ordered grilled cheese and chocolate pudding and cole slaw and V8 and nothing ever tasted so good. Mitch was shocked to hear me say, “You know, that wasn’t so bad. I’m really already starting to forget how much that hurt!” About an hour after that, I started to feel like I’d been put through the ringer, and was so ready to go see my boys. It was such a strange and empty feeling to have given birth so triumphantly but to be without my babies in my arms.
A few hours later, I was allowed to go to the NICU to see my boys. I could not hold them, but I held their hands and stroked their heads and marveled that they had come out of my amazing body. I sang to each of them – “Beautiful Boy,” by John Lennon. Before you go to sleep, say a little prayer, every day in every way, it’s getting better, better, better. Beautiful, beautiful, beautiful, beautiful boy. I’ll never forget Oskar’s little eyes popping open at the sound of my voice.
When it was all said and done, even though almost nothing went according to plan, it worked out exactly like it was supposed to. I had what I can only describe as an amazing, magical labor and birth. Because of my experience, I also feel strongly that beautiful, sacred, soulful birth can happen anywhere: I have had two truly transcendent, at-one-with-the-universe, experiences in my life, and one of them occurred in a brightly lit, sterile OR, on my back, in stirrups, with a literal crowd of people looking on. I felt every second of each passing sensation and now I wouldn’t have wanted it any other way. I ended up getting my “unmedicated” childbirth after all, and I’m really glad now that the epidural didn’t work. In the difficult days after the birth when my boys spent a few weeks growing and getting stronger in the NICU, I thought over and over about how strong and amazing and powerful I was during their birth. If I could do that, then I am capable of anything.
In the time since my boys’ birth, I have become a doula and a childbirth educator. For me, one of the most powerful and important parts of being a birth worker stems from the phrase, “When a baby is born, so is a mother.” I love it so much because that phrase, maybe more than any other, defines who I am now. I was re-born when my boys were born. I’d spent most of my life feeling like I was not very strong, and I’d always been one to give up when something didn’t come easily to me. But our birth – my boys’ and mine – showed me a strength I could never have dreamed I had in me. The experience of giving birth changed me down to my core, and I am forever grateful to those two little souls who illuminated the path toward the rest of my life.
Jess Helle-Morrissey is a doula, a Lamaze-Certified Childbirth Educator, a psychotherapist, a wife, and a mama. She teaches several childbirth education classes at Blooma, including one for families expecting twins, and lives in St. Paul, Minnesota with her three dudes: Mitch, Oskar, and Henry.
Editor’s Note: A version of this story originally appeared on Birth Without Fear.